Clinicopathological Study of Gastrointestinal Endoscopic Biopsies in a Tertiary Care Center
Clinicopathological Study of Gastrointestinal Endoscopic Biopsies in a Tertiary Care Center
Pangeni P. Neera1*, Pradhan A2, Upadhyaya P2, Paudyal P2, Pokhrel S2, Kafle S3, Mudbhari B4
1: Neera P. Pangeni : Senior consultant pathologist, Kanti children hospital, Kathmandu, Nepal
2: Anju Pradhan: Professor, B.P. Koirala institute of health sciences, Dharan, Nepal
Paricha Upadhaya: Professor, B.P. Koirala institute of health sciences, Dharan, Nepal
Punam Paudyal: Additional Professor, B.P. Koirala institute of health sciences, Dharan, Nepal
Sairil Pokhrel: Associate Professor, B.P. Koirala institute of health sciences, Dharan, Nepal
3. Shankar Kafle: Assistant professor, Tribhuvan university teaching Hospital, Maharajgunj, Kathmandu, Nepal
4. Bandana Mudbhari: Consultant pathologist, Nisarga hospital and research center, Dhangadi, Nepal
*Correspondence to: Neera P Pangeni, Kanti children hospital, Maharajgunj, Kathmandu, Nepal.
Copyright
© 2025 Neera P Pangeni. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 26 April 2025
Published: 05 May 2025
Abstract:
Introduction:
Gastrointestinal (GI) mucosal lesions represent a significant health burden. Histopathological study of biopsy specimens is used to confirm endoscopic diagnosis in suspected malignancy or to rule out the endoscopically benign appearing lesions, and, to monitor the course, determine the extent of a disease, responses to therapy and for the early detection of complications.
This study aimed to determine the spectrum of GI mucosal lesions in endoscopic biopsies and correlate endoscopic diagnoses with histopathological findings in Eastern Nepal.
Methods:
A cross-sectional study was conducted at a tertiary care center (B.P. Koirala institute of health sciences, Dharan, Nepal) over a period of 12 months. Endoscopic biopsy samples were received in the pathology department and histopathological examinations were performed. Results were recorded and data analysis included descriptive statistics and diagnostic measurements.
Results:
A total of 45 endoscopic biopsies were analyzed (33 upper GI, 12 lower GI). The mean age of patients was 54.16 years. The most common site for upper GI biopsies was the stomach (37.7%), and for lower GI, it was the colon and rectum (11.11% each). Pain abdomen (86.67%) was the predominant clinical symptom. Histopathological diagnoses varied, with adenocarcinoma being common in both stomach and rectum. The correlation between endoscopic and histopathological diagnoses was evaluated.
Conclusion:
Adenocarcinoma was the most common malignancy in GIT except oesophagus in which squamous cell carcinoma was more common. Esophagitis, gastritis and inflammatory bowel disease were the most common types of non-neoplastic lesion in GIT. This study will be helpful to address the need for a definitive diagnosing tool based on which rapid presumptive diagnosis can be made in suspected cases and adequate treatment can be started accordingly.
Keywords: Benign, diagnosis, endoscopy, histopathology, malignant.
Clinicopathological Study of Gastrointestinal Endoscopic Biopsies in a Tertiary Care Center
Introduction
Gastrointestinal tract disorders are one of the most encountered problems in clinical practice with a high degree of morbidity and mortality.
Gastrointestinal tract can be sited for a wide variety of infections, inflammatory disorders, vascular disorders, mechanical conditions, toxic and physical reactions, including radiation injury and neoplasm. (1)
In the Gastrointestinal tract, the upper gastrointestinal tract consists of the buccal cavity, pharynx, esophagus, stomach and duodenum and the lower gastrointestinal tract includes part of the duodenum below the suspensory muscle and whole of the large intestine. (2)
Mucosal lesions are defined as different degrees of inflammation, erosion, pre-neoplastic and neoplastic lesions of the upper and lower gastrointestinal mucosa originating from the superficial layers/epithelial layer confined to the mucosae or in cases of ulcer and malignancy, penetrating up to the muscularis mucosae. (3)
Incidence of GIT mucosal lesions:
Worldwide gastric adenocarcinoma is the second most common cancer and carcinoma oesophagus is the sixth leading cause of death. (4) In Nepal, gastric carcinoma is the second most common among males. (5) Squamous cell carcinoma of oesophagus is usually seen in the middle third. Squamous cell carcinomas of the oesophagus emerge mainly through a sequence of chronic esophagitis, progressive dysplasia, carcinoma in situ, and finally invasive carcinoma. More than 90% of oesophageal cancers are squamous cell carcinoma or adenocarcinoma, while other types like melanoma, lymphoma, stromal tumours and neuroendocrine tumors are rarely seen. Oesophageal carcinoma shows a wide range of global variation in its incidence and this geographical distribution of cancer can be of great value for generations of epidemiological data. To facilitate diagnosis of different lesions, endoscopy and histology are complementary. (6).
Duodenal biopsies are now commonly performed as a part of Upper GI endoscopic procedure. Common indication for duodenal biopsy includes peptic ulcer disease, symptoms of malabsorption, neoplasia and infectious enteritis. Another common condition affecting duodenum is Celiac disease which is an enteropathy in certain predisposed individuals who have an inappropriate destructive inflammatory reaction against various proline rich proteins including gliadin in wheat, secalin in rye and horde in barley. This reaction may initially begin in proximal duodenum and may later involve entire stomach, small intestine and large intestine. The biopsies should be performed in patients with symptoms and laboratory abnormalities suggestive of
malabsorption and/or nutrient deficiency with the anti-celiac antibodies. Since the clinical presentation of celiac disease is often subtle, it is important that the threshold for biopsy be relatively low. (7)
The concept of a spectrum of histological appearances in chronic inflammatory bowel disease is useful and is convenient for practical assessment. This is particularly true in the early histological appearance of Crohn’s disease when the definitive criteria may not be present. From the point of view of histological assessment, particularly of mucosal biopsies, which are small, the histopathologist is faced with an apparent range of inflammatory changes falling within a continuous spectrum. The accurate histological diagnosis of chronic inflammatory bowel disease is dependent upon either multiple endoscopic biopsies or assessment of a surgically resected specimen. The key reasons for performing biopsies in patients with suspected active ulcerative colitis are to help confirm the diagnosis and to determine the extent of the disease. Knowledge of the latter is important for determining the best management strategy. (8)
In lower Gastrointestinal tract, endoscopy is more often done in patients who suffer from constipation and rectal bleeding although it is important in any kind of early detection of pathologic conditions of the colon. (9) In rare instances, where the gastrointestinal mucosa appears visually normal with endoscopy, the use of biopsy may still be beneficial in determining microscopic disease. In the lower GIT, obtaining biopsies from an endoscopically normal terminal ileum during colonoscopy adds little additional information. However, colonic biopsies of an endoscopically normal colon yield important information on aetiology in patients presenting with chronic diarrhoea. (10)
Most of the lesions are often subtle and cannot be identified during standard White light Endoscopy although the best chances of cure are associated with the early diagnosis. (11) Endoscopic appearances may be valuable in diagnosis but more accurate and detailed information results from histological examination of mucosal biopsy specimens. (12)
In most countries, gastrointestinal diseases are a large burden on the health-care services with GI pathology being a major workload of surgical pathology. There is a wide range of diseases that can affect the lower GIT, ranging from inflammatory to neoplastic lesion. (13) For diagnosis of abnormal mucosa is seen during endoscopy, specimens should be taken of both diseased and adjacent normal appearing mucosa and should be separately labelled to allow staging of the extent and severity of the disease. (14) The advent of fibre optic endoscopy in recent years has enormously extended the diagnostic possibilities in gastroenterology, assessment in certain situations, perhaps especially for small colorectal polyps. (15)
Gastroenterologists rely on the results of the biopsy for correct diagnosis. Therefore, histopathology is an essential complement to endoscopic examination. Hence, the present study aims to determine the spectrum of gastrointestinal lesions by endoscopic biopsy, make definite histopathological diagnosis of various neoplastic and non-neoplastic upper GI tract lesions and associate the endoscopic findings with histomorphology diagnosis.
Materials and Methods
Study Design and Setting:
A cross-sectional, hospital-based study was conducted at B. P. Koirala Institute of Health Sciences (BPKIHS), a tertiary care center in Eastern Nepal.
Inclusion and exclusion criteria: The study included all patients visiting BPKIHS who underwent endoscopy and had biopsy samples taken from gastrointestinal lesions. Patients who refused consent or had open excision biopsies were excluded. A total of 45 cases were included in the study. Patient data, including age, gender, clinical history, endoscopic diagnosis, and lesion site, were recorded.
Histopathological Examination:
Endoscopic biopsy specimens were preserved in 10% formaldehyde, processed, and stained with hematoxylin and eosin (H&E). Special stains were used when necessary. Special stains used were Periodic acid Schiff (PAS) stain to highlight micro-organism, carbohydrate/mucin, Alcian blue for carbohydrate, Combined Alcian blue – PAS technique and Mucicarmine Stain for mucin, Ziehl-Neelsen stain for tubercle bacilli, Gram stain for Gram positive and Gram-negative Bacteria, Giemsa stain to highlight micro-organism (example: Helicobacter pylori). Gastric biopsies were evaluated for mucosa type, surface epithelium, gastric pits, glands, metaplasia, H. pylori status, inflammation, dysplasia, and neoplasia.
Statistical Analysis:
Data was analyzed using SPSS 25. Descriptive statistics included percentages, proportions, ratios, and means. Sensitivity, specificity, positive predictive value (PPV), negative predictive value (NPV), and accuracy were calculated for diagnostic measurements.
Results
Site Distribution of Biopsies:
Of the 45 endoscopic biopsies, 33 were from the upper GI tract and 12 from the lower GI tract. In the upper GI tract, the most common site was the stomach (37.7%), followed by the duodenum (15.5%) and esophagus (13.33%). In the lower GI tract, the colon and rectum were the most common sites (11.11% each). (Fig. 1)
Figure 1: Sitewise distribution of: (A) upper GIT lesions (B) lower GIT lesions
Patient Demographics:
The age ranged from 26 to 85 years, with a mean age of 54.16 years. Most patients were female (57.8%). The most common occupation was housewife (37.8%). The predominant clinical symptom was abdominal pain (86.67%).
Clinical symptoms:
The predominant clinical symptom among the cases who underwent endoscopic biopsies was pain in abdomen (86.67 %) followed by dyspepsia (31.11%), loss of appetite (17.77%), altered bowel habit (17.77%), loss of weight (13.33%), vomiting (8.88%) and burning epigastrium (8.88%). (Fig.2).
In lower Gastrointestinal tract lesions, the most commonly presenting symptom was bleeding per rectum (13.33%) and occult blood positivity was found in 1 case i.e., 2.22%.
Figure 2: Presenting symptoms of the patients.
Endoscopic and Histopathological Findings:
In the upper GI tract, endoscopic findings included suspected malignancy in the esophagus (3 cases), adenocarcinoma in the gastro-oesophageal junction (GEJ) (2 cases), and H. pylori gastritis in the stomach (4 cases). Histopathological diagnoses in the upper GI tract included esophagitis, squamous cell carcinoma, adenocarcinoma, Helicobacter gastritis, and chronic duodenitis. (Fig.3)
Similarly, in the lower GI tract, histopathological diagnoses included adenocarcinoma, Crohn's disease, and ulcerative colitis. (Fig.3)
Figure 3: Histopathological spectrum of GIT mucosal lesions
Association of Endoscopic and Histopathologic Diagnosis:
The association between endoscopic diagnosis and histopathologic diagnosis is tabulated in Table 1. Out of 45 endoscopic mucosal biopsies of GIT, three (3) cases were diagnosed as adenocarcinoma in both endoscopy as well as in histopathology. However, fifteen (15) cases were diagnosed as adenocarcinoma only in histopathology. The malignant cases that were not shown on endoscopy were diagnosed as adenocarcinoma in histopathology alone. Thus, sensitivity for endoscopic diagnosis for adenocarcinoma is 20%, specificity 100%, PPV 100%, NPV 71.43% and accuracy 73.33% which in comparison to histopathological diagnosis is lower.
Patients suspected of malignancy on endoscopy were diagnosed with variable benign and malignant conditions in histopathology. Thirteen (13) cases were suspected of malignancy on endoscopy. Seven (7) out of 13 cases suspected of malignancy in endoscopy were diagnosed as adenocarcinoma, two cases as squamous cell carcinoma, one esophagitis, two chronic non-atrophic gastritis and one chronic duodenitis on histopathological examination. The sensitivity for the endoscopically diagnosed ‘suspicious of malignancy’ was 31.82%, specificity 73.91%, positive predictive value 53.85% and negative predictive value 53.12%. The accuracy of endoscopic diagnosis in this case was only 53.33%. Here, the sensitivity of the endoscopy is very low as compared to histopathology and thus, we conclude that the histopathological examination is always necessary for the definite diagnosis of GIT mucosal lesions.
For benign lesions in upper GIT, Helicobacter gastritis was the commonest on histopathological diagnosis and on comparing the endoscopic diagnosis with the histopathology, specificity of endoscopic diagnosis was 90.00%, while sensitivity was 0.00%, PPV 0.00%, NPV 87.80% and accuracy of 80.00%. This might be because of the microscopic examination of organisms like H. pylori with the special stains which is impossible on endoscopic examination alone.
Similarly, for pangastritis on endoscopy, the specificity of diagnosing chronic non-atrophic gastritis was found to be 97.62 % and accuracy of 91.1% which is quite less compared to the histopathologic diagnosis. One case was diagnosed as erosive gastritis endoscopically but was diagnosed as adenocarcinoma in histopathology. Erosive gastritis when diagnosed on endoscopy, sensitivity was 25%, specificity 100%, PPV 100%, NPV 57.14 % and accuracy of 62.50 %. The sensitivity is found to be very low compared to the gold standard histopathological examination.
Cases diagnosed as eosinophilic gastritis on endoscopy were diagnosed as eosinophilic gastritis on histopathologic examination. The specificity was 97.73%, sensitivity 0.00%, PPV 0.00%, NPV 97.73% and accuracy 95.56%. But these values were found to be very low compared to the histopathologic examination. This might address the lower number of sample size and limited duration of the study leading to the poor association of these methods of diagnosis.
Table 1:Association of Endoscopic and Histopathologic Diagnosis:
|
S.N. |
Diagnosis |
Endoscopic (%) |
Histo-pathology (%) |
Diagnostic test for Endoscopic versus Histopathologic (Histo=gold standard) |
||||
|
Sensitivity (%) |
Specificity (%) |
Positive predictive value |
Negative predictive value |
Accuracy |
||||
|
1. |
Adenocarcinoma |
3 (6.66) |
15(33.33) |
20.00 |
100.00 |
100.00 |
71.43 |
73.33 |
|
2. |
Suspicious of malignancy |
13(28.88) |
22(48.8) |
31.82 |
73.91 |
53.85 |
53.12 |
53.33 |
|
3. |
Dyspepsia under evaluation |
1(2.2%) |
3(6.66) |
0.00 |
97.62 |
0.00 |
93.18 |
91.11 |
|
4. |
Helicobacter gastritis |
4(8.88) |
5(11.11) |
0.00 |
90.00 |
0.00 |
87.80 |
80.00 |
|
5. |
Pangastritis |
1(2.22) |
3(6.66) |
0.00 |
97.62 |
0.00 |
93.18 |
91.11 |
|
6. |
Eosinophilic gastritis |
1(2.22) |
1(2.22) |
0.00 |
97.73 |
0.00 |
97.73 |
95.56 |
|
7. |
Erosive gastritis |
1(2.22) |
4(8.88) |
25.00 |
100.00 |
100.00 |
57.14 |
62.50 |
|
8. |
Ulcer |
5(11.11) |
3(6.66) |
0.00 |
88.10 |
0.00 |
92.50 |
82.22 |
|
9. |
Polyp |
3(6.66) |
1(2.22) |
0.00 |
93.18 |
0.00 |
97.62 |
91.11 |
|
10 |
Gastric Carcinoid |
1(2.22) |
3(6.66) |
0.00 |
97.62 |
0.00 |
93.18 |
91.11 |
|
11 |
Celiac disease |
3(6.66) |
2(4.44) |
0.00 |
93.02 |
0.00 |
95.24 |
88.89 |
|
12 |
Duodenitis |
1(2.22) |
2(4.44) |
0.00 |
97.67 |
0.00 |
95.45 |
93.33 |
|
13 |
Eosinophilic enteritis |
1(2.22) |
2(4.44) |
0.00 |
97.67 |
0.00 |
95.45 |
93.33 |
|
14 |
Crohn’s disease |
2(4.44) |
2(4.44) |
0.00 |
95.35 |
0.00 |
95.35 |
91.11 |
|
15. |
Ulcerative colitis |
3(6.66) |
4(8.88) |
25.00 |
96.08 |
33.33 |
94.23 |
90.91 |
|
16. |
Barrett’s oesophagus |
1(2.22) |
1(2.22) |
0.00 |
97.73 |
0.00 |
97.73 |
95.56 |
|
17. |
Polyposis syndrome |
1(2.22) |
1(2.22) |
0.00 |
97.73 |
0.00 |
97.73 |
95.56 |
The endoscopically diagnosed cases of ulcer had various histopathologic diagnoses. One case was diagnosed as high-grade dysplasia, one case as esophagitis, one case as Helicobacter gastritis and one case as reactive gastropathy in histopathology. Thus, sensitivity is 0.00%, specificity 88.10%, PPV 0.00%, NPV 92.50 % for diagnosis of ulcer in endoscopy which reflects the contradiction of the endoscopy in diagnosing ulcer with that of the gold standard histopathology.
All the three cases diagnosed as polyps on endoscopy were also diagnosed as polyps on histopathology. One case was diagnosed as gastric hyperplastic polyp, one case as fundic gland polyp and one case as Rectal polyp in lower GIT with specificity 93.18%, PPV 0.00%, NPV 97.62%, accuracy 91.1% as compared to the histopathology. Specificity, negative predictive value and accuracy of endoscopy for diagnosing polyp were similar the histopathology. However, the sensitivity and positive predictive values were very low in comparison to the histopathological diagnosis.
One case of gastric carcinoid diagnosed endoscopically was diagnosed as Helicobacter gastritis on histopathology. The specificity of endoscopy in diagnosing this case was 97.62%, PPV 93.18% and accuracy 91.1% but the sensitivity was 0.00% for diagnosing carcinoid endoscopically when compared to the histopathology.
Endoscopically diagnosed 2 cases of Celiac disease were diagnosed as eosinophilic enteritis on histopathology. Thus, the sensitivity was 0.00%, specificity 93.2% and accuracy 88.89%. Out of three cases diagnosed as ulcerative colitis on endoscopy, two cases were diagnosed as ulcerative colitis while one case was diagnosed as adenocarcinoma.
One case of Barrett’s Esophagus diagnosed with endoscopy had similar diagnosis on histopathology. Thus, the sensitivity of endoscopy being 0.00%, specificity 97.73%, PPV 0.00%, NPV 97.73% and accuracy 95.56% when compared to histopathology considering histopathology as the gold standard.
Similarly, for Polyposis Syndrome, the result had 97.73% specificity, 0.00% sensitivity and positive predictive value, negative predictive value was 97.73% and accuracy being 95.56 % for endoscopic diagnosis as compared to the histopathological diagnosis which is lower than that of histopathological diagnosis.
This study showed a poor association between endoscopic diagnosis and histopathologic diagnosis highlighting the fact that histopathological examination has long been considered the gold standard for the diagnosis when abnormal mucosa is seen during the endoscopy.
Discussion
This study aimed to determine the spectrum of gastrointestinal mucosal lesions and correlate endoscopic and histopathological diagnoses. The findings highlight the importance of histopathological examination in the diagnosis of GI mucosal lesions.
Forty-five (45) gastrointestinal mucosal biopsies were included in the study of which 33 were upper GIT biopsies and the rest were lower GIT biopsies.
Socio- demographic profile:
In this study, endoscopic mucosal biopsies were studied on patients of age ranging from 26 to 85 years with the mean age of the patient being 54.16 years. In a study done by Obayo et al showed similar findings where the age of the patients ranged from 18 to 90 years with a mean age of 53.5 years.(16)
In a study by Thapa et al included 80 GIT biopsies. Patients age ranging from 20 years female to 84 years male with a male to female ratio of 1.28: 1.(15) Similarly, in a study conducted by Poudel A et al, in 43 endoscopic biopsies also showed male predominance with 29 males and 14 females. In contrast to these studies, this study showed female predominance with 26 females and 19 males. This difference in gender ratio could be due to shorter duration of the study and lesser number of cases in our study.(17)
Nature of lesions:
Kazi J et al in their study showed correlation between endoscopic and histological diagnosis, conducted in a study of 240 patients who underwent upper gastrointestinal endoscopy for dyspeptic symptoms. The biopsies were taken from oesophagus (158), stomach (193) and duodenum (146). In the correlation with endoscopic diagnosis in 158 oesophageal biopsies, 50 showed no significant
changes, 33 revealed reflux oesophagitis, 8 cases were found to be benign ulcers, 42 had hyperplastic epithelium and 25 carcinomas. There was 100% correlation between the two diagnostic methods when carcinoma was diagnosed on endoscopy. One benign looking ulcer turned out to be malignant on subsequent histology. A single case of carcinoma in situ presented as inflammation on endoscopy. There was a poor correlation between the two diagnostic methods when no significant changes were seen on endoscopy. This study also showed correlation in 193 gastric biopsies, which was good when positive diagnosis was made on endoscopy and poor in negative endoscopy. The lesion most frequently missed was chronic gastritis. One benign looking ulcer was histologically malignant and one large dirty ulcer suspected to be malignant was benign on histology. A distinct and rare clinic-pathological entity eosinophilic gastritis was only diagnosed on histological examination. In 146 duodenal biopsies, the most missed lesion was duodenitis. A case with a polypoidal mass in the duodenum was diagnosed as schwannoma on histology. The nodularity of mucosa seen on endoscopy was found to be produced by Brunner’s gland hyperplasia. (18)
In a retrospective study conducted by Sharma S et al in 50 cases, 58% were male and 42% were females. Out of five cases of erythematous patches diagnosed endoscopically, 40% were found to be normal, 20% as chronic gastritis and 40% were diagnosed as Helicobacter pylori induced gastritis. Out of 16 cases diagnosed as gastric ulcer endoscopically, 25% were found to be normal, 31% cases were diagnosed as chronic gastritis, 25% cases were diagnosed as Helicobacter pyloriinduced gastritis and 6% of cases were diagnosed as ulcer, metaplasia and carcinoma respectively. Similarly, among 12 cases diagnosed as erosion endoscopically, 33% were normal, 33% showed Helicobacter pylori induced chronic gastritis, 25% shows chronic gastritis and 8% showed metaplasia. All 17 of the endoscopically suspected carcinomas correlated histologically as adenocarcinoma, majority of carcinoma presented as an ulcerating fungating growth on endoscopy. (19)
In a similar focused study by Memon et al done in 222 cases of gastric endoscopic biopsies, 40% cases were diagnosed as chronic gastritis with helicobacter pylori followed by chronic non-specific gastritis with activity (35%) and without activity (25%), 11(7.6%) were diagnosed as gastric carcinoma. This study suggested that in case of visible growth or malignancy, the two techniques correlated well with almost similar number of cases detected by each. However, histopathology significantly improved diagnosis of inflammatory lesions. (20)
The increasing use of endoscopy has led to identification of more discernible abnormalities in the stomach including polyps. Gastric polyps encompass a spectrum of pathologic conditions that can vary in histology, neoplastic potential and management. The great majority of polyps detected in the stomach are hyperplastic polyps, fundic gland polyps and adenomatous polyps. (21)
In the study by Islam S et al observed that the most frequent type of polyp was Hyperplastic polyp which is most found in cases with associated Helicobacter pylori infection. (21)
Bhagyalakshmi et al found that most patients with chronic diarrhoea had malignancies of lower GIT seen in the age group of 51-60 years and Inflammatory bowel disease in the age group of 30- 40 years. Most affected segment in this study was recto-sigmoid which is a usual site for ulcerative colitis. 12 out of 13 cases of ulcerative colitis had moderate disease endoscopically with features of erosions, complete loss of vascular pattern, and significant erythema. Remaining case showed only mild mucosal erythema. Histologically all cases showed typical features of ulcerative colitis having marked inflammatory cells in superficial layers and crypt abscesses with neutrophils. (22)
Lansdown et al evaluated patients with gastric dysplasia. On review, only 20 of the 40 patients had true dysplasia. The endoscopic findings of these cases included ulcer, raised tumour or polyp, plaque, atrophic mucosa, irregular mucosa at a gastroenterostomy, deformity of the pyloric canal. The recognition of dysplasia from atypical hyperplasia consequent upon regeneration or inflammatory activity is so bizarre as to give rise to appearances indistinguishable from malignancy. They concluded that it is obligatory for the diagnosis of high-grade dysplasia to be confirmed by a second set of biopsy specimens while the biopsy specimens must be reported on by very experienced pathologists. (23)
Site of biopsy:
In this study, we found most received sample were gastric biopsies comprising 37.7% of the total. Prasaad PR et al in their study also observed 56% of the gastric biopsies.(24) In our study, next common biopsies received were from duodenum (13.33%) followed by esophagus (13.33%) in upper GIT and colonic biopsies in lower GIT accounting for 13.33%. GEJ biopsies accounted for only 6.67% of the total cases while the minimum number of biopsies received was from the Ileum (4.44%). In the studies conducted by Rashmi et al and Prasaad et al, next common specimen was esophageal biopsies (25% and 8% respectively). (1,24)
Clinical presentation:
Pain abdomen was the most common symptom (86.67%) among the patients with GIT mucosal lesions in this study. Memon et al in their study also observed pain abdomen as the commonest presenting symptom(51%) .(20)
Distribution of Oesophageal Lesions:
In our study, among the oesophageal biopsies, 50% were non-neoplastic pathologies and 33.33% were neoplastic lesions. Esophagitis was the most common diagnosis. These results are comparable with the study done by Abilash SC et al in which chronic non-specific esophagitis was the commonest diagnosis.(4)
The neoplastic lesions comprised of squamous cell carcinoma in this study. All the patients diagnosed with carcinoma were found to be above 60 years of age. Similarly in this study, 94% of the patients diagnosed with oesophageal carcinoma were between fifth and sixth decades of life.
In a similar focused study done by Rashmi et al, they found all the cases of oesophageal malignancy as squamous cell carcinoma. (1)
Though the incidence of adenocarcinoma is on the rise in many countries, this study failed to prove that may be partly because of the limited number of patients with oesophageal biopsies.
Distribution of Gastro-oesophageal junction lesions:
Total three (3) cases were identified in gastro-oesophageal junction among which a single case was of chronic non-atrophic gastritis while two cases were diagnosed as adenocarcinoma.
Distribution of Gastric Lesions:
In the present study, among the 17 gastric biopsies, 13 cases were diagnosed as benign while 4 cases were diagnosed as malignant i.e., 76.5 % and 23.5 % respectively. The incidence of benign and malignant conditions is like the studies done by Thapa et al and Rashmi et al. (15,1)
Thapa et al, in their study done on gastric biopsies found that non-neoplastic lesions constituted 67.5% and neoplastic lesions being 37.5 % only. Most common non-neoplastic lesion noted was mild chronic gastritis (27.5%) followed by chronic active gastritis and H.pylori was present in 16.25 % of the cases.(15)
Helicobacter pylori gastritis was the most encountered inflammatory lesions in gastric biopsies in this study (29.4%). All the cases revealed the presence of Helicobacter pylori on Giemsa stain. However, chronic non-atrophic gastritis and eosinophilic gastritis comprised of 5.9 % each.
Similarly in a study done by Prasaad PR et al, H.pylori infection was the most common cause of chronic gastritis. They have also stated that in underdeveloped countries, H.pylori infection manifests as multifocal atrophic gastritis which has patchy involvement of the pylorus, body and cardiac mucosa warranting the need for multiple site representative biopsies for the proper diagnosis of H.pylori gastritis.(24)
One case each of fundic gland polyp and gastric hyperplastic polyp was identified in this study which was similar to the studies done by Yanik et al. and Umana et al. (9,13)
Eosinophilic gastritis is a distinct and rare clinic-pathological entity. In our study, one single case was diagnosed as eosinophilic gastritis in endoscopy which on histopathology turned out to be chronic non-atrophic gastritis. Similarly, in a study done by Kazi J et al, it was diagnosed only on histological examination.(18)
We observed a single case of gastric xanthelasma. Similarly , in a study conducted by Parsad PR et al, one of the gastric biopsy showed Xanthelasma.(24)
In our study, 3 cases were diagnosed as adenocarcinoma in endoscopy, and all were confirmed by histopathology as adenocarcinoma. This was in comparison to study conducted by Kazi J et al and Thapa et al. (15,18)
Adenocarcinoma was diagnosed in cases having age above 60 years in this study. In a study done by Thapa et al, adenocarcinoma was the most common gastric malignancy which is comparable with this study. Gastric carcinoma is uncommon before the age of 40 years but thereafter, its incidence increases progressively with increasing age, peaking in the seventh decade of life . (15)
Distribution of Duodenal Lesions:
Duodenum has a rich rapidly regenerating epithelial lining which can easily be affected by any inflammatory insult .(20)
We received only seven cases of endoscopic biopsy for histopathologic diagnosis involving the upper two parts of the duodenum. Two (2) cases had chronic duodenitis. 1 case was diagnosed as peptic duodenitis and the rest of the two cases revealed features of eosinophilic enteritis and celiac sprue each.
This is comparable to the previous study done by Abilash SC et al in which out of 60 duodenal biopsies, 43 patients showed nonspecific duodenitis, 6 cases of duodenal ulcer, 5 cases of polyp and 1 case of celiac disease.(4)
However, cases of duodenal polyp were not identified in this study as compared to other studies.
Distribution of Lower GIT Lesions:
Out of twelve (12) lower GIT biopsies received, 5 cases were of inflammatory bowel diseases (41.67%), 1 case of inflammatory rectal polyp (8.3%) and six (6) cases were of adenocarcinoma (50%).
A total of five (5) cases were diagnosed as Inflammatory bowel disease. Three (60%) cases were of ulcerative colitis and 2(40%) cases were diagnosed with Crohn’s disease.
The peak age group for the Inflammatory bowel disease was < 60 years’ age group, for both the males and females. In the study done by Umana et al, the peak age group for IBD was 50-59 years for both the males and females. The endoscopic findings were also similar to this study.(13)
In a similar study done by Umana et al, out of 18 cases , 11 (61.1%) were diagnosed as ulcerative colitis, 6 (33.33%) cases were of Crohn’s disease and 1 (5.6%) case was of indeterminate colitis.(13)
A single inflammatory rectal polyp was identified on histopathologic examination which is similar to the study conducted by Umana et al where the polyps were frequently located in the rectum.(13) This ,however, differs from what was seen in the study by Choanozoan MK, et al where the predominant location was the ascending colon and caecum.(26)
Clark JC et al stated that polyps usually occur in a similar site of the colon, where we have a higher occurrence of colorectal carcinoma. This concurs with what is seen in this study i.e. polyps and colorectal carcinoma both found to be mostly located in the rectum.(27)
Malignant lesions in lower GIT:
The malignant lesions were the predominant lesions seen in lower GIT (50%).This concurs with the findings of Umana et al where colorectal adenocarcinoma was the predominant lesion diagnosed accounting for 50 % of the total lower GI endoscopic biopsies.(13)
In this study, one case of colonic adenocarcinoma was below 60 years of age group.
Similarly, Umana et al found that the first peak age observed for colorectal carcinoma was between 50-59 years of age group.(13)
However, in this study majority of the colorectal adenocarcinomas belonged to above 60years of age group. This finding was slightly different from what was reported by Abdulkareem et al where the peak age was in the 4th and 5th decade. This may be attributed to the fact that the colorectal screening programs were more established and standardized in those centers and thus, the early detection of the disease.(28)
Colorectal carcinoma was the commonest malignant condition in lower GIT in this study. This frequency (50%) of the total lower GIT biopsies is indeed higher in comparison to the incidence rate in previous years in our part of the world. With passing generations and the accompanying lifestyle changes, there is an associated increased incidence of colorectal carcinoma. (22)
Hence, this study attempts to disseminate the above data reflecting the increasing incidence of colorectal carcinoma in our part of the world. This highlights the fact that the colorectal screening programmes should be emphasized and put into practice at the community level, and we should think of programmes targeted at creating local level health awareness.
In this study, out of the 45 pathological lesions diagnosed, inflammatory lesions (49%) were the most common followed in order by malignancies (33.33%), inflammatory bowel diseases (11%) and polyps (6.7%).
A study conducted at T. M. medical college by Joshi et al also showed similar results in which the inflammatory lesions were the most common diagnosis. However, in contrast to our study, they found out polyps and inflammatory bowel diseases being most common than malignancies. (29)
This variation of data may be attributed to the socio-demographic profile of the people in various parts of the world and the standardized screening programmes in more developed countries.
Association between Endoscopic diagnosis and histopathologic diagnosis:
Our study showed a poor association between endoscopic diagnosis and histopathologic diagnosis in majority of cases.
There was a good concordance among both these diagnostic methods in diagnosing adenocarcinoma in 3 cases only. However, 15 cases were diagnosed as adenocarcinoma in histopathology only. Thus, the sensitivity of endoscopy for diagnosing adenocarcinoma was lower in comparison to the histopathologic diagnosis.
This highlights the fact that in diagnosing the malignancies, the presence of muscularis mucosae layer is essential in the GIT mucosal biopsies to look for the invasion but the tiny endoscopic biopsies in most of the time fail to represent the entire pathologic condition of the site and the lesion in the mucosa.
Our study also showed a poor association between endoscopy and histopathology in diagnosing various inflammatory lesions which is similar to a study conducted by Guindy et al.(30)
In our study, we observed that in case of visible growth or malignancy, the two methods of diagnosis correlated well. However, histopathology significantly improved the diagnosis of endoscopically suspected malignancies and confirmed 15 cases of adenocarcinoma, and these were not diagnosed in endoscopy.
This was in coherent with the study done by Niknam et al in which histologic premalignant lesions were significantly higher in patients with abnormal endoscopy. However, in contrast they also showed that 6.8% of the total cases with normal gastric endoscopy had histologic premalignant lesions. We did not receive any biopsies from the patients with normal endoscopy in our study.(31)
Thus, we conclude that the individual accuracy and sensitivity of these two methods of diagnosis in diagnosing any GIT lesions is attributed firstly to the endoscopy operator’s ability to target the site of pathology and submit the representative biopsy and then most importantly the reporting histopathologist’s vigilant observation, experience and knowledge in gastro-enter pathology.
Conclusion
Gastrointestinal tract is a common site of diverse lesions; both neoplastic and non-neoplastic. This study provides valuable data on the spectrum of GI lesions in Eastern Nepal, which will give the overall view of the disease burden in the society. This study will add some facts and figures to the literature, which will serve as a reference material for those willing to do similar research in the future. However, the study is limited by the smaller sample size and short duration of study period.
Acknowledgement: None
Conflict of interest: There is not any conflict of interest.
Please click here to view complete article
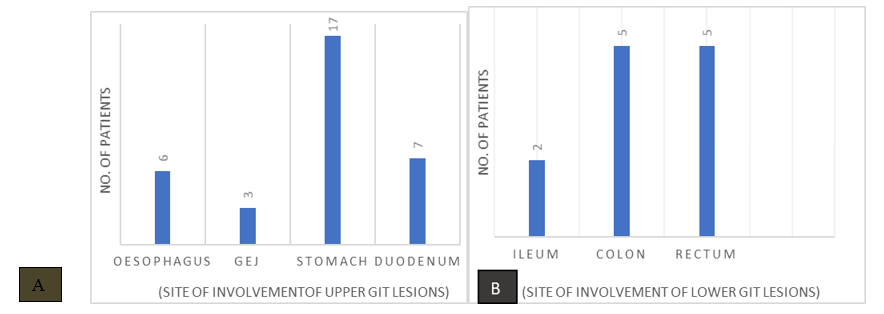
Figure 1
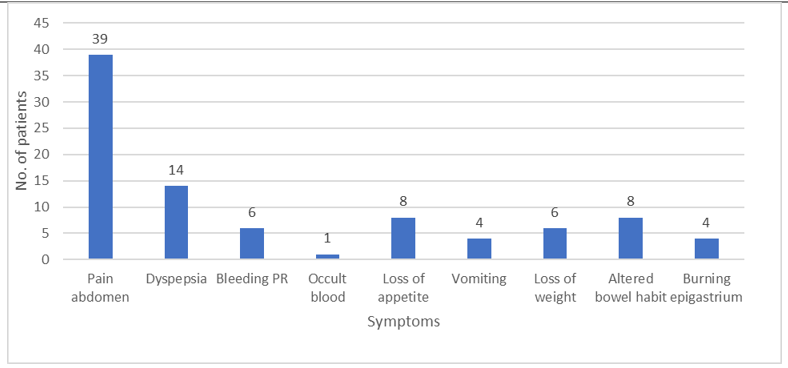
Figure 2
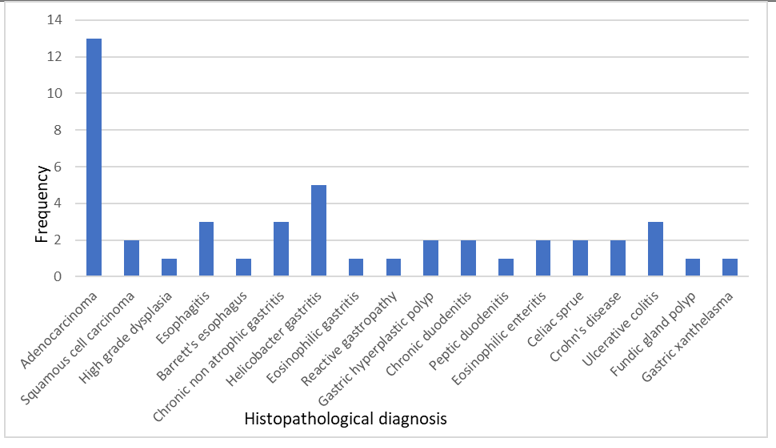
Figure 3
