Heterotopic Pregnancy
Heterotopic Pregnancy
Taha A B.1*, Jamieson A.2
1) Obstetrics and Gynaecology Registrar, Princess Royal Maternity Hospital, Glasgow, Scotland, UK.
2) Consultant Obstetrician & Gynaecologist, Princess Royal Maternity Hospital, Glasgow, Scotland, UK.
*Correspondence to: Aisha Babikir Taha, MBBS, MD, MRCOG.
Copyright
© 2025 Aisha Babikir Taha. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 07 July 2025
Published: 06 Aug 2025
Abstract
Background:
Heterotopic pregnancy refers to the simultaneous occurrence of intrauterine and ectopic gestations, a rare but potentially life-threatening condition. Though historically uncommon in spontaneous pregnancies, its incidence has increased with the use of assisted reproductive technologies (ART), such as in vitro fertilization (IVF). Early diagnosis is challenging due to overlapping symptoms with other gynecologic or non-gynecologic conditions.
Case Presentation:
We report a rare case of heterotopic pregnancy in a 39-year-old primigravida who conceived via IVF. At 11 weeks of gestation, she presented with vaginal bleeding and mild abdominal pain. Ultrasound examination revealed a viable intrauterine pregnancy alongside a left adnexal ectopic mass with hemoperitoneum. She underwent emergency laparoscopic left salpingectomy. Histopathological evaluation confirmed tubal ectopic pregnancy. The intrauterine pregnancy remained viable and progressed normally.
Conclusion:
This case underscores the importance of maintaining a high index of suspicion for heterotopic pregnancy, particularly in patients undergoing assisted reproduction. Timely diagnosis and surgical intervention are crucial to prevent maternal morbidity while preserving the intrauterine pregnancy.
Keywords:
Heterotopic pregnancy, ectopic pregnancy, intrauterine pregnancy, IVF, assisted reproductive technology, laparoscopy
Heterotopic Pregnancy
Introduction
Heterotopic pregnancy is the presence of multiple gestations, one being present in the uterine cavity and the other extra-uterine, commonly in the fallopian tube and uncommonly in the cervix or ovary. It is rare, occurring in about 1 in 30,000 spontaneous pregnancies, but potentially life-threatening. The risk rises to 1-3% in Advanced Reproductive Therapy and IVF. [1,2] Diagnosis can still sometimes be overwhelming due to the presence of an Intrauterine Pregnancy. [3]
Heterotopic pregnancies are usually diagnosed from 5 to 34 weeks of gestation.[4] Tal et al.[5] reported that 70% of the heterotopic pregnancies were diagnosed between 5 and 8 weeks of gestation, 20% between 9 and 10 weeks and only 10% after the 11th week. [5] Presentation is vague and up to 50% of patients are asymptomatic. [8] The differential diagnoses of Heterotopic Pregnancy include: Acute Abdominal pain, Flare-up of Endometritis, ovarian cyst accident, miscarriage and non-gynaecological causes such as acute appendicitis and severe Urinary Tract Infection. [2]
The Risk factors include: Previous ectopic, Advanced Reproductive Therapy and In Vitro Fertilization, pelvic surgeries, Pelvic Inflammatory Disease, Intrauterine Contraceptive Devices and smoking. However, in most cases, no risk factors were found [2]
Heterotopic Pregnancy may be discovered late, increasing the risk of considerable life-threatening haemorrhage and hypovolemia as a consequence of the Ectopic Pregnancy rupture. [7]
Case Presentation
We report a heterotopic pregnancy in a 39-year-old primigravida with a spontaneous pregnancy. She had an NHS booking scan at 11 weeks which showed intrauterine pregnancy with normal right adnexa, left adnexa ‘not seen’.
She then had a private ultrasound scan which showed a heterotopic pregnancy and was therefore referred to the hospital.
Upon presentation, she had brownish vaginal discharge and mild abdominal pain.
This patient had a background history of endometriosis and had x2 laparoscopic ovarian cystectomies in the past. She had a blocked left tube seen on a Hycose test in Italy before. Her Serum HCG was negative 2 days before the Hycose.
Her abdomen was mildly tender on examination with voluntary guarding. A transvaginal Ultrasound showed a viable intrauterine pregnancy at 12+4 weeks and another viable left tubal ectopic pregnancy of 11 weeks + 6 days gestation. She underwent laparoscopic surgery where a small amount of bleeding was seen in the abdomen, and an ectopic mass in the left adnexa. This mass was removed safely using Ligasure. The procedure was uncomplicated with 100mls of blood loss. She had a bedside USS post-op op which confirmed a viable intrauterinepregnancy.
Figure 1
Figure 2
Figure 3
Figure 4
Discussion
Heterotopic pregnancy is the presence of multiple gestations, one being present in the uterine cavity and the other extra-uterine, commonly in the fallopian tube and uncommonly in the cervix or ovary. It is rare, occurring in about 1 in 30,000 spontaneous pregnancies, but potentially life-threatening. The risk rises to 1-3% in Advanced Reproductive Therapy and IVF. [1,2]. 1/100 when associated with in vitro fertilization, and 1/900 when using clomiphene citrate. [9]
A detailed history and physical examination are importance to explore all risk factors related to heterotopic pregnancy.
Heterotopic Pregnancy may be discovered late, increasing the risk of considerable life-threatening haemorrhage and hypovolemia as a consequence of the Ectopic Pregnancy rupture. [7]
The Risk factors include: Previous ectopic, Advanced Reproductive Therapy and In Vitro Fertilization, pelvic surgeries, Pelvic Inflammatory Disease, Intrauterine Contraceptive Devices and smoking. However, in most cases, no risk factors were found [2]
β-hCG's level is not useful for of heterotopic pregnancy's diagnosis. Intrauterine pregnancy masks all underlying β-hCG changes from ectopic pregnancy and vice versa. [10]
Diagnosis can still sometimes be overwhelming due to the presence of an Intrauterine Pregnancy. [3]
Maintaining a high index of suspicion is critical for the diagnosis of heterotopic pregnancy.
Heterotopic pregnancies are usually diagnosed from 5 to 34 weeks of gestation.[4] Tal et al.[5] reported that 70% of the heterotopic pregnancies were diagnosed between 5 and 8 weeks of gestation, 20% between 9 and 10 weeks and only 10% after the 11th week. [5] Presentation is vague and up to 50% of patients are asymptomatic. [8]
The differential diagnoses of Heterotopic Pregnancy include: Acute Abdominal pain, Flare-up of Endometritis, ovarian cyst accident, miscarriage and non-gynaecological causes such as acute appendicitis and severe Urinary Tract Infection. [2]
Combination of history, examination and ultrasound can give suggestion of heterotopic pregnancy. Definitive diagnosis can be made with laparoscopy which can be used as treatment option as well.
In hemodynamically stable and asymptomatic women, expectant management could be considered, the main advantage of expectant management is avoiding all potential complications related to the surgical management. However, expectant management should not be considered in patients with a viable or large ectopic pregnancy due to the high risk of rupture of the ectopic pregnancy. [11]
The laparoscopic approach has been proven to be an effective and safe option in managing early ectopic pregnancy. Surgical management by laparoscopic salpingectomy in a tubal ectopic pregnancy is generally a safe procedure with no increase in fetal loss rate in the IUP. Surgical management has the advantage of complete removal of the ectopic pregnancy mass. However, the outcomes and the complexity of the surgery can vary depending on the location of the ectopic component of the ectopic pregnancy. [13]
In this case, the decision was to proceed with laparoscopy, with the possibility of laparotomy. The decision was appropriate given the patient presentation; was in pain, had viable heterotopic pregnancy, thus laparcoscopic salpingectomy was safe and appropriate.
She continues to have ongoing normal pregnancy and is 29+wks now.
Conclusion
An early pregnancy transvaginal ultrasound scan should be offered to women at high risk for Ectopic Pregnancy. When performing an ultrasound in early pregnancy, Heterotopic Pregnancy should always be suspected in patients with an adnexal mass, even in the absence of risk factors. Clinicians must be alert to the fact that confirming an intrauterine pregnancy clinically or by ultrasound does not exclude the coexistence of an Ectopic Pregnancy. A high index of suspicion in women is needed for early and timely diagnosis. Laparoscopic Salpingectomy can result in a favourable and successful obstetrical outcome.
References
1. Bright D. A., Gaupp F. B. Heterotopic pregnancy: a reevaluation. The Journal of the American Board of Family Practice .1990;3(2):125–128.
2. Barrenetxea G., Barinaga-Rementeria L., Lopez de Larruzea A., Agirregoikoa J. A., Mandiola M., Carbonero K. Heterotopic pregnancy: two cases and a comparative review. Fertility and Sterility. 2007;87(2):417.e9–417.e15. doi:10.1016/j.fertnstert.2006.05.085
3. Li X. H., Ouyang Y., Lu G. X. Value of transvaginal sonography in diagnosing heterotopic pregnancy after in-vitro fertilisation with embryo transfer. Ultrasound in Obstetrics and Gynaecology
4. Varras M, Akrivis c, Hadjopoulos G, Antoniou N. Heterotopic pregnancy in a natural conception cycle presenting with tubal rupture: a case report and review of the literature. Eur J Obstet Gynecol Reprod Biol. 2003;106:79–82
5. Tal J, Haddad S, Gordon N, Timor-Tritsch I. Heterotopic pregnancy after ovulation induction and assisted reproductive technologies: a literature review from 1971 to 1993. Fertil Steril. 1996;66:1–124.
6. Yu Y., Xu W., Xie Z., Huang Q., Li S. Management and outcome of 25 heterotopic pregnancies in Zhejiang, China.European Journal of Obstetrics, Gynecology, and Reproductive Biology .
7. Avitabile N. C., Kaban N. L., Siadecki S. D., Lewiss R. E., Saul T. Two cases of heterotopic Pregnancy. Journal of Ultrasound in Medicine
8. Elsayed, S., Farah, N., & Anglim, M. (2023). Heterotopic Pregnancy: Case Series and Review of Diagnosis and Management. Case Reports in Obstetrics and Gynecology, 2023, 2124191. https://doi.org/10.1155/2023/2124191
9. Bataille P., Reynard A., Ducarme G. Spontaneous heterotopic triplets – a review of literature. J. Gynecol. Obstet. Hum. Reprod. 2017;46(8):657–659. doi: 10.1016/j.jogoh.2017.05.008.
10. J.-B. Li L.-Z. Kong J.-B. Yang G. Niu L. Fan J.-Z. Huang S Chen Management of Heterotopic Pregnancy: Experience From 1 Tertiary Medical Center Medicine Observational study.
11.Hirose M., Nomura T., Wakuda K., Ishiguro T., Yoshida Y. Combined intrauterine and ovarian pregnancy: a case report. Asia-Oceania Journal of Obstetrics and Gynaecology . 1994;20(1):25–29. doi: 10.1111/j.1447-0756.1994.tb00416.x.
13. Avitabile N. C., Kaban N. L., Siadecki S. D., Lewiss R. E., Saul T. Two cases of heterotopic Pregnancy. Journal of Ultrasound in Medicine . 2015;34(3):527–530. doi: 10.7863/ultra.34.3.527.

Figure 1
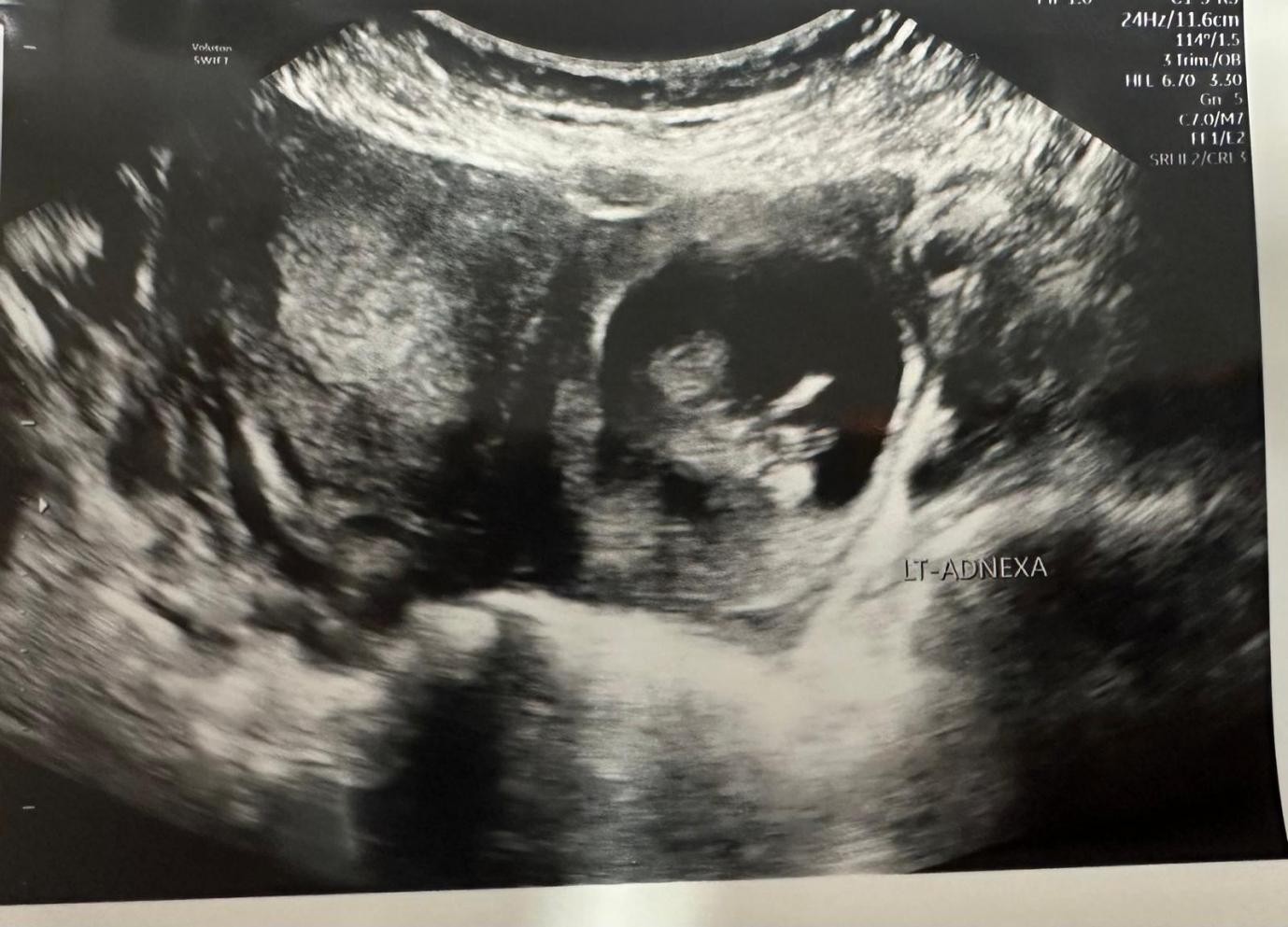
Figure 2

Figure 3

Figure 4
