Critical Care Nurses' Compliance and Barriers toward Ventilator-Associated Pneumonia Prevention Guidelines
Critical Care Nurses' Compliance and Barriers toward Ventilator-Associated Pneumonia Prevention Guidelines
Eidah Alrashdi1*, Nagwa Ibrahim Abbas Ghoneim2, Naimah Naif Ayidh Al Salem3, Norah Al Mutairi4, Mesfer Alrashidi5
1. Nursing specialist in Maternity hospital
2. Lecturer of Critical Care and Emergency Nursing, Faculty of Nursing, Tanta University, Egypt.
Assist prof, Nursing Department, Applied Medical Sciences College, UHB, SA. (orcid.org/0000-0003-1385-4024)
4,5. General Nurse Specialist, Hafer Albatin, Saudi Arabia.
*Correspondence to: Eidah Alrashdi, SA.
Copyright
© 2025: Eidah Alrashdi. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 08 Sep 2025
Published: 22 Sep 2025
ABSTRACT
Background Background: Ventilator-associated pneumonia (VAP) is a significant and preventable health condition affecting thousands of patients annually. This condition can lead to severe complications and is potentially fatal. Despite the availability of numerous evidence-based preventive measures performed by nurses to reduce its incidence, compliance remains a challenge. This study aimed to evaluate critical care nurses' compliance with and barriers to ventilator-associated pneumonia prevention guidelines.
Methods: A cross-sectional study was conducted in the intensive care unit of King Khaled Hospital, KSA. Convenience sampling was utilized proportionally according to the number of staff in each department, resulting in a sample of 62 ICU nurses. Data was collected using a self-reported questionnaire consisting of socio-demographic characteristics of ICU nurses, compliance with VAP prevention guidelines assessment, and barriers to compliance assessment. Statistical analysis was performed using descriptive and inferential statistics to determine the relationships between knowledge levels and socio-demographic variables. Ethical approval was obtained.
Results: The study revealed that most participants were young, predominantly female, and held a bachelor degree, with 59.7% aged between 20–30 years and 82.3% being female. Most were Saudi nationals (87.1%), and nearly 70% had 1–5 years of ICU experience. Approximately 64.5% of participants worked in ICUs with 10–15 beds, but 83.9% had not received prior training on ventilator-associated pneumonia (VAP) prevention guidelines. Knowledge gaps were significant, with only 46.8% of nurses demonstrating satisfactory knowledge levels. Correct responses to key VAP prevention elements, such as recommended bed positioning (16.1%) and antibiotic course duration (30.6%), were particularly low. Statistical analysis indicated significant relationships between knowledge levels and factors like age, education, experience, and training, but no significant relationship with gender or job title. Barriers to compliance included nursing staff shortages, inadequate education, lack of supplies, and insufficient time for evidence-based procedures, showing the need for targeted interventions to enhance training, institutional support, and resource availability.
Conclusion The majority of nurses demonstrated unsatisfactory knowledge regarding VAP prevention guidelines, with statistically significant associations between knowledge and certain socio-demographic characteristics. The study recommends implementing educational and training programs to improve nurses' knowledge and adherence to VAP prevention guidelines, ultimately aiming to reduce the incidence of VAP among ventilated patients in the Saudi healthcare system.
Keywords: Critical care nurses' compliance - barriers - ventilator-associated pneumonia - prevention guidelines.
Critical Care Nurses' Compliance and Barriers toward Ventilator-Associated Pneumonia Prevention Guidelines
Introduction
Ventilator-associated pneumonia (VAP) is a significant healthcare issue, impacting thousands of patients annually and resulting in increased morbidity, mortality, and healthcare costs. This preventable infection is associated with mechanical ventilation, a life-saving intervention frequently used in intensive care units (ICUs). VAP accounts for approximately one-third of nosocomial pneumonia cases in ICUs, with the Centers for Disease Control and Prevention (CDC) reporting that 32% of pneumonia cases in U.S. acute care hospitals in 2015 were linked to ventilator use. Its impact extends beyond patient outcomes, as it increases ventilator dependency, prolongs ICU stays, and raises healthcare expenses (Fernando et al., 2020; Papazian, Klompas, & Luyt, 2020).
VAP is defined as a pulmonary infection occurring in mechanically ventilated patients (MVPs) after at least 48 hours of endotracheal intubation. The prevalence of VAP is alarmingly high, ranging from 9% to 27%. Intubated patients are particularly vulnerable during the first five days of ventilation, when the risk of developing VAP is highest. Globally, the incidence of VAP varies, with developing countries experiencing the highest rates. In the United States, VAP incidence is reported to be between 1.1 and 7.4 episodes per 1,000 ventilator-days in adult ICUs. However, the International Nosocomial Infection Control Consortium (INICC) reported a significantly higher incidence rate of 14.7 episodes per 1,000 ventilator-days in 43 developing countries, including regions in Latin America, Asia, Africa, and Saudi Arabia (Mohamed et al., 2023).
Studies in Saudi Arabia showed the critical nature of VAP in ICUs. Research analyzing infection rates across 12 Ministry of Health hospitals revealed that VAP was the most common deviceassociated healthcare-associated infection (DA-HAI), accounting for 57.4% of such cases. Further analysis by the INICC in five Saudi cities between 2013 and 2015 reported an incidence rate of 7.5 episodes per 1,000 ventilator-days. These statistics illustrate the disparity in VAP incidence globally, which is influenced by differences in surveillance models, healthcare resources, and prevention practices (Gaid et al., 2018; Abdulla et al., 2023). The financial and clinical burden of VAP is profound; in Saudi Arabia, each episode of VAP is associated with an additional $40,000 in hospital costs, an average ICU stay extension of 17.5 days, and an excess mortality rate of 31.8% (Gaspar et al., 2023).
The complications of mechanical ventilation are multifaceted, with VAP being one of the most significant. The endotracheal tube (ETT) serves as a conduit for bacterial migration from the oral cavity to the lungs, reducing salivary flow, impairing mucus clearance, and inhibiting the cough reflex. These factors contribute to bacterial colonization and the development of VAP. This risk is heightened in patients requiring intubation for conditions such as airway protection, surgeries, or reduced consciousness (Weber, 2023). The consequences are severe; patients who develop VAP have a five to ten times higher risk of acquiring nosocomial infections and experience increased mortality rates, with death occurring in 33% of cases (Mumtaz et al., 2023).
Efforts to prevent VAP in critical care settings have led to the development of various strategies, including elevating the head of the bed, providing oral care, administering prophylactic antibiotics, and adhering to care bundles. These measures have been shown to decrease ventilator dependency and ICU stays. Notably, VAP bundles, which combine multiple evidence-based interventions, are particularly effective. The duration of mechanical ventilation remains the most significant risk factor, and reducing ventilator days is key to prevention (Coelho, Moniz, Guerreiro, & Póvoa, 2023; Safavi et al., 2023). Oral care, a cornerstone of VAP prevention, has been shown to significantly reduce respiratory tract infections when performed consistently and correctly. Research showed the importance of nurse education, technique, and compliance in the successful implementation of these measures (Alotaibi, 2023).
Despite the availability of clinical guidelines, adherence to VAP prevention strategies remains inconsistent. Barriers such as institutional differences, limited awareness, and variability in training contribute to this gap between ideal and current practice. In Saudi Arabia, the challenges of implementing these guidelines are further compounded by resource constraints and diverse healthcare settings. Addressing these issues is essential for improving nurse compliance and ensuring consistent application of evidence-based measures (Alotaibi, 2023; Wolfensberger et al., 2023). Nurses are at the forefront of VAP prevention, given their direct contact with patients and their responsibility for implementing the majority of interventions.
The global burden of VAP, coupled with its clinical and financial consequences, showed the importance of effective prevention strategies. In ICUs, where patients are most vulnerable, ensuring adherence to evidence-based guidelines is critical. This study aimed to evaluate the compliance of critical care nurses with VAP prevention measures and identify the barriers hindering adherence. By bridging the gap between knowledge and practice, healthcare institutions can significantly reduce the incidence of VAP, improve patient outcomes, and optimize healthcare resources. Empowering nurses through education, institutional support, and standardized guidelines is essential in combating this preventable yet impactful infection.
Methods
Study Design The research employed a cross-sectional study design, which allowed for the analysis of relationships among variables without establishing causality. This design is particularly useful for capturing data at a single point in time to assess critical care nurses’ compliance with ventilator-associated pneumonia (VAP) prevention guidelines and the barriers they encounter in implementing these measures (Setyawati, Lu, Liu, & Liang, 2020).
Study Setting This study was conducted in the intensive care unit (ICU) of King Khaled Hospital, located in Hafr Al-Batin, Saudi Arabia. King Khaled Hospital is a leading healthcare facility in the region, providing a wide array of medical services to the city and its surrounding areas. The hospital offers specialties such as emergency care, general medicine, surgery, pediatrics, obstetrics and gynecology, orthopedics, cardiology, and neurology. Equipped with state-of-the-art medical technology, the hospital is designed to deliver high-quality, patient-centered care.
Sampling The target population for the study comprised staff nurses working in the ICU of King Khaled Hospital who had at least one year of experience in bedside patient care. A convenience sampling method was utilized, proportionally representing staff from different departments. Inclusion criteria ensured a diverse sample, encompassing nurses of all qualifications, varying years of experience, different nationalities, and both genders. Participation was voluntary, with only those willing to partake in the study included in the sample.
Tools of Study A self-reported questionnaire was employed to collect data, divided into three distinct sections. The first section focused on the sociodemographic characteristics of ICU nurses, including age, gender, nationality, marital status, education level, position, years of ICU experience, the type of ICU, the number of beds, and prior education on ventilator management and VAP prevention. The second section assessed nurses’ compliance with VAP prevention guidelines through 11 multiple-choice questions covering knowledge of definitions, causes, guidelines, and complications. Responses were scored, with one point for each correct answer, yielding a total score of 11. Compliance was categorized as good (75–95%), average (60–74%), or poor (below 60%). The third section investigated barriers to guideline adherence, utilizing an 18-item Likert scale with responses ranging from strongly disagree to strongly agree. This section explored challenges related to knowledge gaps, workload, institutional factors, communication, and patient safety concerns.
Tool Validity and Reliability The validity of the questionnaire was assessed by five experts in the critical care nursing field, achieving a Content Validity Index (CVI) score of 97%. The reliability of the tool was measured using Cronbach's alpha, with a coefficient of 0.57. Adjustments and refinements were made based on feedback from the experts and results of a pilot study to enhance the clarity and applicability of the tools.
Pilot Study A pilot study was conducted with 10% of the target population to test the clarity and usability of the research tools. This phase also helped estimate the time required for data collection and identify potential challenges. Participants from the pilot study were excluded from the main research to ensure data integrity.
Compliance with VAP Prevention Guidelines The study revealed varying levels of compliance with VAP prevention practices among ICU nurses. High compliance rates were observed for practices such as head-of-bed elevation (70–100%) and oral care with chlorhexidine (60–100%). Moderate compliance was noted for daily sedation vacations and readiness-to-extubate assessments (60–88%). Lower compliance rates were recorded for interventions such as subglottic suctioning (30–75%), ventilator circuit changes only when necessary (40–80%), and the use of endotracheal tubes with subglottic suction ports (30–80%).
Barriers to VAP Prevention Guideline Adherence The study evaluated the presence and level of barriers affecting adherence to ventilator- The study identified and evaluated key barriers affecting adherence to ventilator-associated pneumonia (VAP) prevention guidelines, categorized into knowledge gaps, workload challenges, institutional factors, communication issues, and patient safety concerns. Knowledge deficits emerged as a primary barrier, with nurses lacking familiarity with current guidelines and uncertainty about certain interventions' effectiveness. Workload pressures, such as heavy patient assignments and high acuity levels in ICUs, further limited time for implementing preventive measures. Institutional shortcomings, including inadequate supplies like subglottic suction catheters and the absence of clear protocols, compounded the problem. Poor interdisciplinary collaboration and disagreements between nurses and physicians regarding certain practices also hindered adherence. Additionally, nurses expressed concerns that some measures, such as sedation holds, might compromise patient safety or comfort, creating reluctance to implement them. These findings showed the need for targeted strategies to address these barriers, including education, improved staffing, clearer institutional policies, and enhanced communication, to improve adherence and patient outcomes in ICU settings.
Statistical Analysis Data were coded, entered, and analyzed using the Statistical Package for Social Sciences (SPSS) version 23. Statistical techniques were applied to achieve the study’s objectives, with results presented in a structured format. Sociodemographic data were visualized through figures, while tables and charts were used to depict nurses’ knowledge of VAP prevention and barriers to compliance. This comprehensive approach provided insights into the factors influencing adherence to VAP prevention guidelines and showed areas for improvement in ICU nursing practices.
Ethical Considerations Ethical approval was obtained from the Ethics Committee of the High Institute of Public Health. Participants received comprehensive information about the study’s purpose, benefits, risks, and voluntary nature. Written consent was secured before participation, and nurses were informed of their right to withdraw at any time without consequences. The study ensured anonymity, confidentiality, and privacy throughout the research process, safeguarding the safety and rights of all participants. Following official approval from King Khaled Hospital’s administration, data collection was conducted over a designated period. The researcher personally explained the study’s objectives and procedures to participants and clarified how to complete the questionnaires. Data was gathered during morning shifts, with interviews conducted at times convenient for the nurses.
Results
Socio-Demographic Characteristics of Participants
The socio-demographic characteristics of the critical care nurses are detailed in Table 1. The age ranged from 20 to 45 years. The majority, 37 nurses (59.7%), were within the 20–30-year age group, followed by 23 nurses (37.1%) in the 30–40-year range. Only a small proportion of nurses (3.2%) were aged 36–45 years, and 3.6% were 40 years or older. Regarding gender, the overwhelming majority of participants were female (82.3%). In terms of education, 75.2% of the nurses held a bachelor's degree. Most participants (87.1%) were Saudi nationals, with 40.3% being single.
Concerning their professional roles, 82.3% held the position of staff nurse. A significant portion of the nurses (69.4%) had between 1–5 years of experience, and 72.6% worked in ICUs. Additionally, 64.5% worked in ICUs with 10–15 beds. These characteristics showed the varied yet predominantly young, educated, and female composition of the critical care nursing workforce at the studied hospital.
Table (1): Percentage distribution of the studied critical care nurses according to their sociodemographic data (n=62)
|
Participants characteristics |
N |
% |
|
Age |
|
|
|
20–30 Years |
37 |
59.7% |
|
30–40 Years |
23 |
37.1% |
|
≥40 Years |
2
|
3.2%
|
|
Gender |
|
|
|
Male |
11 |
17.7% |
|
Female |
51 |
82.3% |
|
Nationality |
|
|
|
Saudi |
54 |
87.1% |
|
Non-Saudi |
8 |
12.9% |
|
Religion |
|
|
|
Muslim |
59 |
95.2% |
|
Non-Muslim |
3 |
4.8% |
|
Marital Status |
|
|
|
Single |
25 |
40.3% |
|
Married |
35 |
56.5% |
|
Divorced/Widowed |
2 |
3.2% |
|
Job Title/Current Position |
|
|
|
Staff Nurse |
51 |
82.3% |
|
In-Charge Nurse |
10 |
16.1% |
|
Head Nurse |
1 |
1.6% |
|
Years of Experience |
|
|
|
1–5 Years |
43 |
69.4% |
|
6–10 Years |
10 |
16.1% |
|
>10 Years |
9 |
14.5% |
|
Type of Critical Care Unit |
|
|
|
ICU |
45 |
72.6% |
|
CCU |
6 |
9.7% |
|
PICU |
3 |
4.8% |
|
NICU |
8
|
12.9%
|
|
Number of Beds in ICU |
|
|
|
10–15 Beds |
40 |
64.5% |
|
16–20 Beds |
14 |
22.6% |
|
>20 Beds |
8 |
12.9% |
Figure (1): Percentage distribution of the studied critical care nurses according to their educational qualifications (n=62)
Figure (2) shows previous training programs regarding ventilator-associated pneumonia prevention guidelines that 83.9% of nurses weren’t attend any previous training program regarding ventilator-associated pneumonia prevention guidelines.
Nurses’ Knowledge of VAP Prevention Guidelines
Table 2 provides insights into critical care nurses' knowledge of VAP prevention guidelines. The results revealed significant gaps in understanding some key aspects of VAP prevention. The lowest percentages of correct answers were observed for questions related to the recommended bed position for ventilated patients (16.1%), the recommended course of antibiotic therapy for VAP patients (30.6%), and the common complications associated with ventilators (30.6%). These findings suggest a notable lack of awareness about crucial elements of VAP prevention among the nurses. The mean total knowledge score was 5.03±2.13, indicating an overall moderate level of knowledge.
Table 2: Critical care nurses’ knowledge related to VAP prevention guidelines.
|
ITEMS |
Correct answer |
||
|
N |
% |
||
|
1. What does VAP stand for. |
43 |
69.4 |
|
|
2. The duration in which pneumonia can develop in patient on mechanical ventilation. |
49 |
79.0 |
|
|
3. Diagnosis of ventilator-associated pneumonia |
31 |
50.0 |
|
|
4. The blood test that identifies the microorganisms causing ventilation associated pneumonia. |
38 |
61.3 |
|
|
5. Cause of ventilation associated pneumonia. |
35 |
56.5 |
|
|
6. Method for preventing ventilation associated pneumonia. |
26 |
41.9 |
|
|
7. Sign of early development (96 hours) of ventilation associated pneumonia |
23 |
37.1 |
|
|
8. The current guidance of the ventilation association pneumonia recommended for patient bed position |
10 |
16.1 |
|
|
9. Current guidelines recommend for a course of antibiotics therapy for patients with ventilator associated pneumonia. |
19 |
30.6 |
|
|
10. The common complication of ventilators associated pneumonia. |
19 |
30.6 |
|
|
11. Prevent meager of ventilator associated pneumonia. |
24 |
38.7 |
|
|
Total score |
5.03±2.13 |
||
Figure (3) shows level of nurses’ knowledge related to VAP prevention guidelines. It was shown from the figure that more than half (53.2%) had unsatisfactory level while 46.8% were had satisfactory level.
Relationship Between Socio-Demographic Characteristics and Knowledge Levels
Table 3 explores the relationship between socio-demographic characteristics and knowledge of VAP prevention guidelines. A statistically significant relationship was identified between knowledge and several factors, including age (p=0.001), educational level (p=0.037), years of experience (p=0.018), and participation in previous training programs (p=0.021). These findings showed the importance of experience, education, and prior training in enhancing nurses' knowledge of VAP prevention. Conversely, no significant relationship was observed between knowledge levels and other demographic characteristics, such as gender and job title (p > 0.05). This indicates that while professional development plays a critical role in improving knowledge, other variables, such as gender or current position, may not significantly influence understanding of VAP prevention.
Table 3: Relation between sociodemographic characteristics of the studied and level of knowledge related to VAP prevention guidelines.
|
Participants characteristics |
Knowledge level |
Test of significant |
|
Unsatisfactory knowledge Satisfactory knowledge |
||
|
N % N % |
X2 (P) |
|
Age |
|
|
|
|
|
|
20-30 Years |
28 |
75.7 |
9 |
24.3 |
10.925 |
|
30-40 Years |
5 |
21.7 |
18 |
78.3 |
0.001** |
|
≥40 Years |
0 |
0.0 |
2 |
100.0 |
|
|
Gender |
|
|
|
|
|
|
Male |
26 |
51.0 |
25 |
49.0 |
0.582 |
|
Female |
7 |
63.6 |
4 |
36.4 |
0.445 |
|
Educational level |
|
|
|
|
|
|
Diploma |
5 |
71.4 |
2 |
28.6 |
6.598 |
|
Bachelor |
27 |
57.4 |
20 |
42.6 |
0.037* |
|
Master |
1 |
12.5 |
7 |
87.5 |
|
|
Job title/Current position |
|
|
|
|
|
|
Staff nurse |
30 |
58.8 |
21 |
41.2 |
3.947 |
|
In charger nurse |
3 |
30.0 |
7 |
70.0 |
0.139 |
|
Head nurse |
0 |
0.0 |
1 |
100.0 |
|
|
Years of experience |
|
|
|
|
|
|
1-5 yrs. |
27 |
62.8 |
16 |
37.2 |
8.034 |
|
6-10 yrs. |
5 |
50.0 |
5 |
50.0 |
0.018* |
|
> 10 yrs. |
1 |
11.1 |
8 |
88.9 |
|
|
Previous training program |
|
|
|
|
|
|
Yes |
2 |
20.0 |
8 |
80.0 |
5.287 |
|
No |
31 |
59.6 |
21 |
40.4 |
0.021* |
Barriers to Compliance with VAP Prevention Guidelines
Table 4 showed the barriers to compliance with VAP prevention guidelines. In terms of administrative and resource-related barriers, the most significant challenges included the unavailability of hospital cost-control policies (mean=2.31±1.1) and a lack of professional role models and guidance (mean=1.84±1.12). These administrative issues showed systemic factors that hinder adherence to VAP prevention protocols.
Nursing staff-related barriers were prominent, with a shortage of nursing staff (mean=3.11±1.15) being the most critical challenge. Additional barriers included insufficient education on VAP prevention during university training (mean=2.44±1.18), fear of unpredictable adverse effects and undesirable patient outcomes (mean=2.63±1.22), and the absence of continuous education on VAP prevention (mean=2.71±1.14). These findings suggest that a lack of foundational and ongoing education, compounded by staffing shortages, significantly affects compliance.
Research-related barriers were also evident, with forgetfulness among nurses in performing evidence-based procedures (mean=2.48±1.2) and insufficient time to implement evidence-based practices (mean=2.82±1.19) emerging as key challenges. These results showed the pressing need for better time management strategies and institutional support to increase adherence to evidencebased practices.
Table 4: Critical care nurses’ barriers related to the compliance with VAP prevention guidelines.
|
Barrier |
Strongly disagree |
Disagree |
Agree |
Strongly agree |
Mean±SD |
||||||||||||
|
N % |
N % |
N % |
N % |
||||||||||||||
|
Administration of Resources |
|
|
|
|
|
|
|
|
|
||||||||
|
Unavailable sterile gloves |
39 |
62.9 |
10 |
16.1 |
10 |
16.1 |
3 |
4.8 |
1.63±0.93 |
||||||||
|
Unavailable personal protective equipment |
37 |
59.7 |
11 |
17.7 |
11 |
17.7 |
3 |
4.8 |
1.68±0.94 |
||||||||
|
Unavailable closed suction system |
36 |
58.1 |
12 |
19.4 |
12 |
19.4 |
2 |
3.2 |
1.68±0.9 |
||||||||
|
Unavailable kinetic beds |
34 |
54.8 |
13 |
21.0 |
13 |
21.0 |
2 |
3.2 |
1.73±0.91 |
||||||||
|
Unavailability of written protocols for VAP Prevention. |
44 |
71.0 |
8 |
12.9 |
8 |
12.9 |
2 |
3.2 |
1.48±0.84 |
||||||||
|
Unavailable Hospitals' cost control policy. |
22 |
35.5 |
7 |
11.3 |
25 |
40.3 |
8 |
12.9 |
2.31±1.1 |
||||||||
|
Lack of professional role model and guidance. |
36 |
58.1 |
8 |
12.9 |
10 |
16.1 |
8 |
12.9 |
1.84±1.12 |
||||||||
|
Nursing staff |
|
|
|
|
|
|
|
|
|
||||||||
|
Shortage of nursing staff |
10 |
16.1 |
7 |
11.3 |
11 |
17.7 |
34 |
54.8 |
3.11±1.15 |
||||||||
|
Lack of education in the university about the VAP prevention. |
22 |
35.5 |
4 |
6.5 |
23 |
37.1 |
13 |
21.0 |
2.44±1.18 |
||||||||
|
Nurses lack required skill. |
43 |
69.4 |
10 |
16.1 |
5 |
8.1 |
4 |
6.5 |
1.52±0.9 |
||||||||
|
Lack of patient cooperation. |
40 |
64.5 |
10 |
16.1 |
8 |
12.9 |
4 |
6.5 |
1.61±0.95 |
||||||||
|
Some VAP prevention procedures are not nurses' responsibility. |
37 |
59.7 |
10 |
16.1 |
9 |
14.5 |
6 |
9.7 |
1.74±1.04 |
||||||||
|
Fear of unpredictable adverse effect and undesirable patient outcome |
16 |
25.8 |
13 |
21.0 |
11 |
17.7 |
22 |
35.5 |
2.63±1.22 |
||||||||
|
No continuous education on VA |
11 |
17.7 |
18 |
29.0 |
11 |
17.7 |
22 |
35.5 |
2.71±1.14 |
||||||||
|
Research |
|
|
|
|
|
|
|
|
|
||||||||
|
Practice in ICUs not based on research finding. |
22 |
35.5 |
15 |
24.2 |
11 |
17.7 |
14 |
22.6 |
2.27±1.18 |
||||||||
|
Some research findings contradict nurses' previous education. |
37 |
59.7 |
9 |
14.5 |
5 |
8.1 |
11 |
17.7 |
1.84±1.18 |
||||||||
|
Nurse forgetfulness to perform some evidence-based procedure. |
22 |
35.5 |
8 |
12.9 |
12 |
19.4 |
20 |
32.3 |
2.48±1.28 |
||||||||
|
Nurses do you are not having enough time to perform evidence-based procedure. |
15 |
24.2 |
5 |
8.1 |
18 |
29.0 |
24 |
38.7 |
2.82±1.19 |
||||||||
Discussion
Intubation of the trachea and invasive mechanical ventilation (MV) were critical interventions in intensive care units (ICUs) that saved the lives of severely ill patients. However, these procedures were associated with complications, most notably ventilator-associated pneumonia (VAP). VAP was defined as a parenchymal lung infection occurring 48 hours or more after intubation and initiation of MV, without prior symptoms of lower respiratory infection. It remained a significant healthcare-associated infection (HAI), impacting patient safety worldwide (Alreshidi et al., 2024). Rates of VAP varied widely among countries, which showed the importance of evaluating critical care nurses’ compliance with prevention guidelines and identifying barriers to adherence.
Our study revealed that most critical care nurses were aged 20–30 years, predominantly female, and held bachelor’s degrees. Most nurses were Saudi nationals, single, and worked as staff nurses with 1–5 years of ICU experience in units with 10–15 beds. These findings aligned with AlSayaghi (2021), who reported higher compliance with VAP prevention guidelines among nurses working in ICUs with similar bed capacities, potentially due to optimal nurse-patient ratios and manageable workloads. Conversely, Alkubati et al. (2023) found similar demographic characteristics among Yemeni ICU nurses but noted that less than half had received training on VAP prevention, reflecting disparities in access to educational opportunities.
Our results indicated that most nurses had not attended prior training programs on VAP prevention. This finding was consistent with the foundational study by Labeau et al. (2007), which reported an average knowledge score of 45% among critical care nurses. The validated questionnaire used in their study was later modified and applied in multiple settings, consistently revealing low knowledge scores. For example, Branco et al. (2020) observed a mean knowledge score of 5 (range 3–8) out of 10 among ICU nurses and practitioners, while Saini et al. (2017) reported a mean score of 3.86 ± 1.56. Despite years of evidence supporting ventilator bundle (VB) implementation, knowledge gaps and poor adherence persisted globally.
Similarly, Abad et al. found significant knowledge gaps and inconsistent adherence to VB components, including oral care and peptic ulcer prophylaxis. However, adherence to these components approached 100% in some settings where standardized instructions were incorporated into treatment charts (World Health Organization, 2008). This suggested that implementing a checklist or daily treatment chart could standardize practices and improve compliance, as demonstrated by the WHO surgical safety checklist.
The compliance rate in our study was 85.9%, exceeding rates reported in Spain (Jam et al., 2017) and several regions in Europe and the Middle East (Ricard et al., 2012). This higher compliance rate in Saudi Arabia was consistent with findings by Aloush et al. (2018) and El-Saed et al. (2016), who reported better adherence to VAP prevention bundles in Saudi hospitals compared to Jordanian and Egyptian counterparts. Mogyoródi et al. (2023) also observed that compliance was highest immediately after guideline implementation but declined over time, showed the importance of regular refresher training to sustain adherence.
Educational interventions were shown to enhance compliance with VAP prevention strategies. Álvarez-Lerma and Sánchez García (2018) and Branco et al. (2020) demonstrated that structured educational programs improved adherence to VB and reduced VAP incidence. Bouadma et al. (2010) reported a 51% reduction in VAP incidence following a two-year continuous education program, which included bedside skill demonstrations and feedback. However, Saini et al. (2017) showed that short-term training alone did not lead to sustained reductions in VAP incidence; instead, intensive and ongoing efforts were necessary.
Our study identified significant barriers to compliance, including resource constraints, staffing shortages, inadequate education, and fear of adverse patient outcomes. These findings were in line with Aloush et al. (2020) and Jansson et al. (2018), who reported that cost-control policies, insufficient staffing, and lack of training hindered adherence to VAP prevention guidelines. Additionally, Alotaibi (2023) showed the role of time constraints, supply shortages, and patient conditions in limiting compliance with oral hygiene, head-of-bed elevation, and hand hygiene protocols.
Systemic interventions, such as increasing ICU staffing and implementing cost-effective strategies, were suggested to alleviate these barriers. The use of a checklist-based approach appeared to bridge the gap between knowledge and practice, ensuring consistent adherence to VB components. For instance, Pandey and Uniyal (2011) noted that using subglottic drainage tubes or closed suction systems, though not evaluated in this study, could further enhance prevention efforts.
Our findings showed the need for targeted interventions to address knowledge gaps, improve training, and mitigate barriers to VAP prevention. Incorporating a checklist into daily treatment charts, as suggested by Labeau et al. (2007) and modeled after the WHO surgical safety checklist, could standardize practices and improve compliance. Continuous education programs, such as those described by Bouadma et al. (2010), should be implemented to sustain long-term adherence.
Furthermore, periodic refresher training and multidisciplinary collaboration were deemed essential for success. Future research should investigate systemic factors influencing compliance and explore innovative educational strategies tailored to ICU settings. Addressing these issues would not only reduce VAP incidence but also contribute to safer, more efficient ICU care worldwide.
Conclusion
The study concluded that most of the nurses surveyed demonstrated unsatisfactory knowledge levels regarding ventilator-associated pneumonia (VAP) prevention guidelines. Significant associations were identified between knowledge levels and sociodemographic factors such as age, education, years of experience, and prior training, whereas no significant relationship was found with gender or job title. Key barriers to adherence included excessive workloads, inadequate supplies, and insufficient experience in ICU settings. To address these challenges, the study recommends the implementation of structured educational and training programs to improve nurses’ knowledge and adherence to evidence-based VAP prevention guidelines. Enhancing knowledge and compliance is essential for reducing the incidence of VAP among mechanically ventilated patients in Saudi Arabia.
The findings showed the importance of regular evaluation of healthcare workers’ (HCWs) knowledge to increase awareness and encourage adherence to updated guidelines. Institutions should organize frequent in-service training programs focusing on evidence-based VAP prevention measures. Written care protocols for mechanically ventilated patients should be distributed across hospitals and regularly updated to reflect current evidence. Additionally, medical and nursing curricula should be revised to include the latest guidelines for VAP prevention. However, limitations such as the sample size, lack of a control group, short observation period, variability in operator experience, and cost considerations may affect the generalizability and interpretation of these findings, warranting further research to validate and expand upon these results.
Reference:
1. Alkubati, S. A., Saghir, S. A., Al-Sayaghi, K. M., Alhariri, A., & Al-Areefi, M. (2023). Healthcare workers’ knowledge of evidence-based guidelines for prevention of ventilator-associated pneumonia in Hodeida, Yemen. Journal of Basic and Clinical Physiology and Pharmacology, 34(3), 321-327.
2. Alotaibi, N. E. D. (2023). Factors influencing intensive care nurses' adherence to 'Prevention of Ventilator-Associated Pneumonia' clinical practice guidelines in Saudi Arabia: A mixed-methods study (Doctoral dissertation).
3. Aloush, S. M., & Al?Rawajfa, O. M. (2020). Prevention of ventilator?associated pneumonia in intensive care units: Barriers and compliance. International Journal of Nursing Practice, 26(5), e12838.
4. Aloush, S. M., Abdelkader, F. A., Al-Sayaghi, K., Tawalbeh, L. I., Suliman, M., Al Bashtawy, M., & Shaban, I. (2018). Compliance of nurses and hospitals with ventilator-associated pneumonia prevention guidelines: A Middle Eastern survey. Journal of Nursing Care Quality, 33(3), E8-E14.
5. Alreshidi, M. S., AlRashidi, F. A., Tuppal, C. P., Al Rashidi, N., Prudencio, D. A. M., Villagracia, R. W. A., & Villagracia, H. N. (2024). Nurses’ knowledge on the prevention of ventilatorassociated pneumonia (VAP) among critically ill patients: A one-group pretest-posttest design. Nurse Media Journal of Nursing, 14(1), 65-73.
6. Al-Sayaghi, K. M. (2021). Critical care nurses' compliance and barriers toward ventilatorassociated pneumonia prevention guidelines: Cross-sectional survey. Journal of Taibah University Medical Sciences, 16(2), 274-282.
7. Álvarez-Lerma, F., & Sánchez García, M., Task Force of Experts for Project "Zero VAP" in Spain. (2018). The multimodal approach for ventilator-associated pneumonia prevention - Requirements for nationwide implementation. Annals of Translational Medicine, 6(21), 420. https://doi.org/10.21037/atm.2018.08.40
8. Bouadma, L., Mourvillier, B., Deiler, V., Le Corre, B., Lolom, I., Regnier, B., et al. (2010). A multifaceted program to prevent ventilator-associated pneumonia: Impact on compliance with preventive measures. Critical Care Medicine, 38(3), 789–796. https://doi.org/10.1097/CCM.0b013e3181ce21af
9. Branco, A., Lourencone, E., Monteiro, A., Fonseca, J., Blatt, C., & Aquino, R. (2020). Education to prevent ventilator-associated pneumonia in intensive care unit. Revista Brasileira de Enfermagem, 73(6), e20190477. https://doi.org/10.1590/0034-7167-2019-0477
10. Coelho, L., Moniz, P., Guerreiro, G., & Póvoa, P. (2023). Airway and respiratory devices in the prevention of ventilator-associated pneumonia. Medicina, 59(2), 199.
11. El-Saed, A., Al-Jardani, A., Althaqafi, A., Alansari, H., Alsalman, J., Al Maskari, Z., ... & Balkhy, H. H. (2016). Ventilator-associated pneumonia rates in critical care units in three Arabian Gulf countries: A 6-year surveillance study. American Journal of Infection Control, 44(7), 794-798.
12. Fernando, S. M., Tran, A., Cheng, W., Klompas, M., Kyeremanteng, K., Mehta, S., ... & Rochwerg, B. (2020). Diagnosis of ventilator-associated pneumonia in critically ill adult patients—a systematic review and meta-analysis. Intensive Care Medicine, 46(5), 1170-1179.
13. Gaid, A., Assiri, A., McNabb, S., & Banjar, W. (2018). Device-associated nosocomial infection in general hospitals, Kingdom of Saudi Arabia, 2013–2016. Journal of Epidemiology and Global Health, 7(Suppl), S35–S40.
14. Gaspar, M. D. D. R., Rinaldi, E. C. A., Mello, R. G., Dos Santos, F. A., Nadal, J. M., Cabral, L. P. A., & Farago, P. V. (2023). Impact of evidence-based bundles on ventilator-associated pneumonia prevention: A systematic review. The Journal of Infection in Developing Countries, 17(2), 194201.
15. Jam, R., Hernández, O., Mesquida, J., Turégano, C., Carrillo, E., Pedragosa, R., ... & DelgadoHito, P. (2017). Nursing workload and adherence to non-pharmacological measures in the prevention of ventilator-associated pneumonia: A pilot study. Enfermería Intensiva (English Edition, 28(4), 178-186.
16. Jansson, M. M., Syrjälä, H. P., Talman, K., Meriläinen, M. H., & Ala-Kokko, T. I. (2018). Critical care nurses' knowledge of, adherence to, and barriers toward institution-specific ventilator bundle. American Journal of Infection Control, 46(9), 1051-1056.
17. Mogyoródi, B., Skultéti, D., Mez?csáti, M., Dunai, E., Magyar, P., Hermann, C., ... & Iványi, Z. D. (2023). Effect of an educational intervention on compliance with care bundle items to prevent ventilator-associated pneumonia. Intensive and Critical Care Medicine.
18. Mohamed, H. T., Alenezi, W. A. F., Alanzi, M. A. A., Alsuqub, F. I. S., Alhazmi, S. A. S., & Alhazmi, O. M. M. (2023). Prevalence of ventilator-associated pneumonia in children admitted to pediatric intensive care units in the Middle East: A systematic review. Cureus, 15(12).
19. Mumtaz, H., Saqib, M., Khan, W., Ismail, S. M., Sohail, H., Muneeb, M., & Sheikh, S. S. (2023). Ventilator-associated pneumonia in intensive care unit patients: A systematic review. Annals of Medicine and Surgery, 85(6), 2932-2939.
20.Pandey, R., & Uniyal, B. (2011). Comparing influence of intermittent subglottic secretions drainage with/without closed suction systems on the incidence of ventilator-associated pneumonia.
21. Indian Journal of Critical Care Medicine, 15(3), 168–172. https://doi.org/10.4103/09725229.84902
22.Papazian, L., Klompas, M., & Luyt, C. E. (2020). Ventilator-associated pneumonia in adults: A narrative review. Intensive Care Medicine, 46(5), 888-906.
23. Patil, H. V., & Patil, V. C. (2017). Incidence, bacteriology, and clinical outcome of ventilatorassociated pneumonia at tertiary care hospital. Journal of Natural Science, Biology, and Medicine, 8(1), 46.
24. Ricard, J. D., Conti, G., Boucherie, M., Hormann, C., Poelaert, J., Quintel, M., ... & Torres, A. (2012). A European survey of nosocomial infection control and hospital-acquired pneumonia prevention practices. Journal of Infection, 65(4), 285-291.
25. Safavi, A., Molavynejad, S., Rashidi, M., Asadizaker, M., & Maraghi, E. (2023). The effect of an infection control guideline on the incidence of ventilator-associated pneumonia in patients admitted to the intensive care units. BMC Infectious Diseases, 23(1), 198.
26. Saini, V., Gandhi, K., Kaur, K., & Yaddanapudi, L. N. (2017). Effect of intensive education and training of nurses on ventilator-associated pneumonia and central line-associated bloodstream infection incidence in intensive care unit at a tertiary care center in North India. Indian Journal of Critical Care Medicine, 21(11), 779–782. https://doi.org/10.4103/ijccm.IJCCM_259_17
27. Setyawati, A. D., Yu-Ying, L., Chieh-Yu, L., & Shu-Yuan, L. (2020). Disaster knowledge, skills, and preparedness among nurses in Bengkulu, Indonesia: A descriptive correlational survey study. Journal of Emergency Nursing, 46(5), 633-641. https://doi.org/10.1016/j.jen.2020.04.004
28. Weber, J. (2023). Registered nurse education on prevention of ventilator-associated pneumonia in an urban midwestern intensive care unit.
29.Wolfensberger, A., Clack, L., von Felten, S., Hesse, M. F., Saleschus, D., Meier, M. T., ... & Sax, H. (2023). Prevention of non-ventilator-associated hospital-acquired pneumonia in Switzerland: A type 2 hybrid effectiveness–implementation trial. The Lancet Infectious Diseases, 23(7), 836-846.
30.World Health Organization. (2008). Safe Surgery Saves Lives. Retrieved October 16, 2015, from http://www.who.int/patientsafety/safesurgery/ss_checklist/en/index.htm.
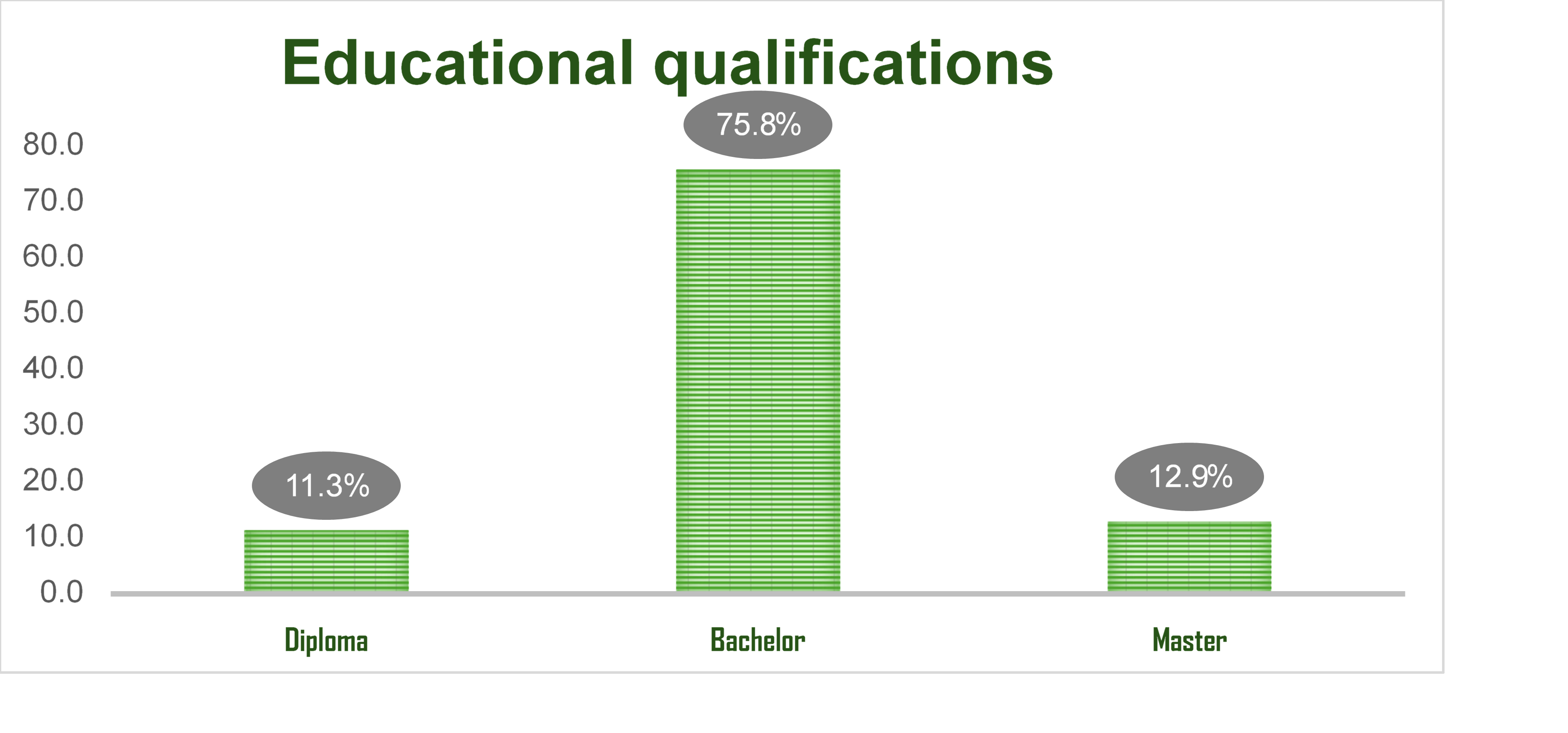
Figure 1
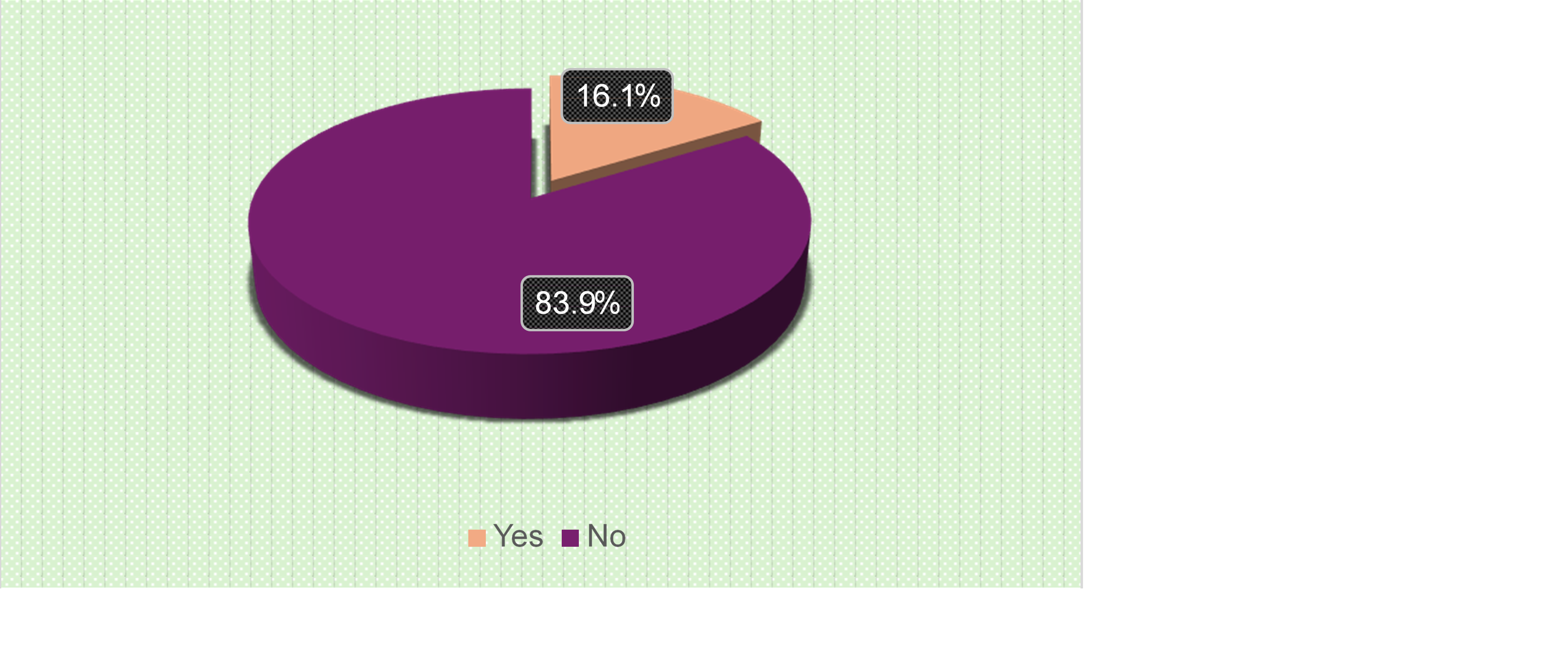
Figure 2
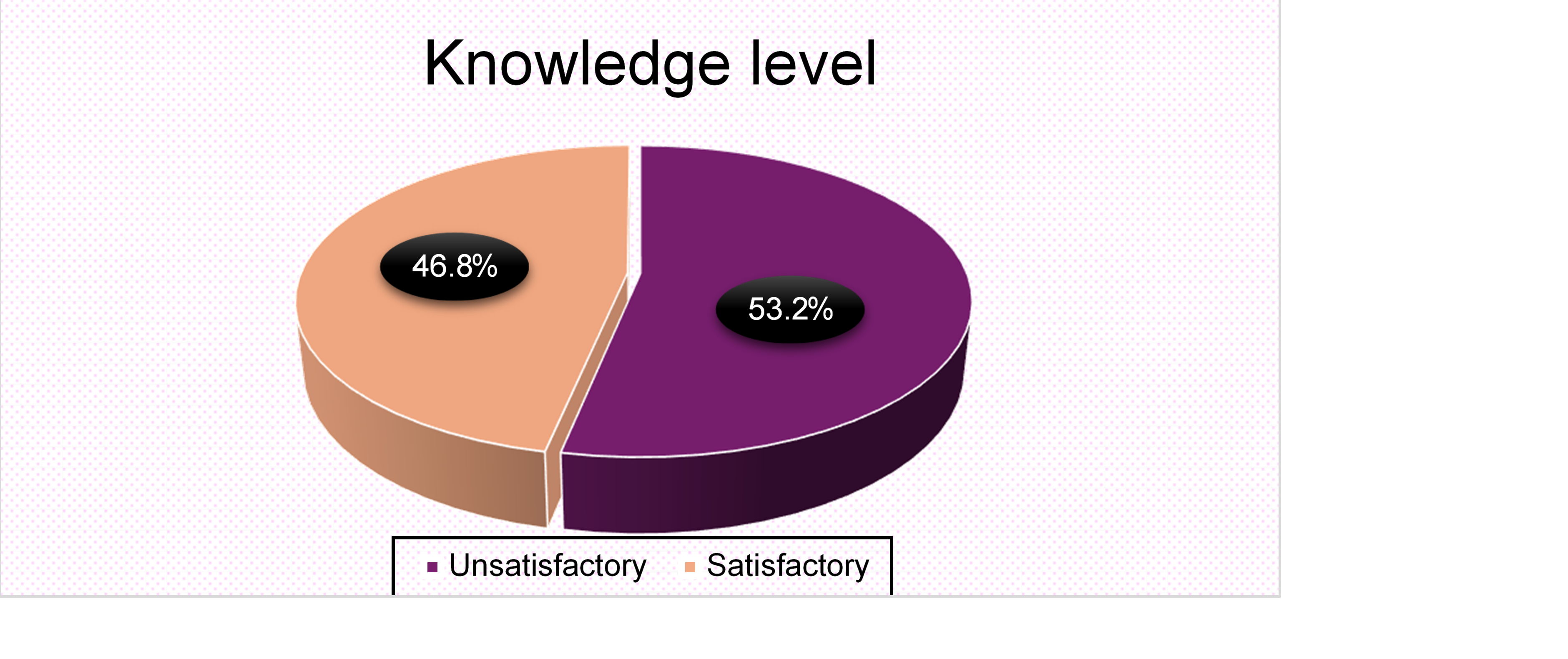
Figure 3
